Canadians have grown accustomed to having personal and community health information at their fingertips, via devices and apps that literally put our health in our hands. For the most part these are welcome innovations. But what if you’re someone who has no access, or limited access, to technology? It’s a conundrum with growing implications for social equity and community health.
At the best of times, obtaining the full range of our personal health data (as opposed to the quick vital statistics available through fitness apps) can be challenging. Clients must navigate a variety of different systems, often using a different portal for each provider. That’s not a surprise, given a system organized around providers rather than patients, as Canada’s is. It’s a system that can and should change, to put patients at its centre.
For while the problem of access is partly structural, embedded in technology, there are core issues of policy, governance and accountability at play here as well — each subject to reform. Provinces and territories, which administer health care in Canada, must necessarily be partners in such reforms. This work, complex and politically fraught though it will be, should begin now.
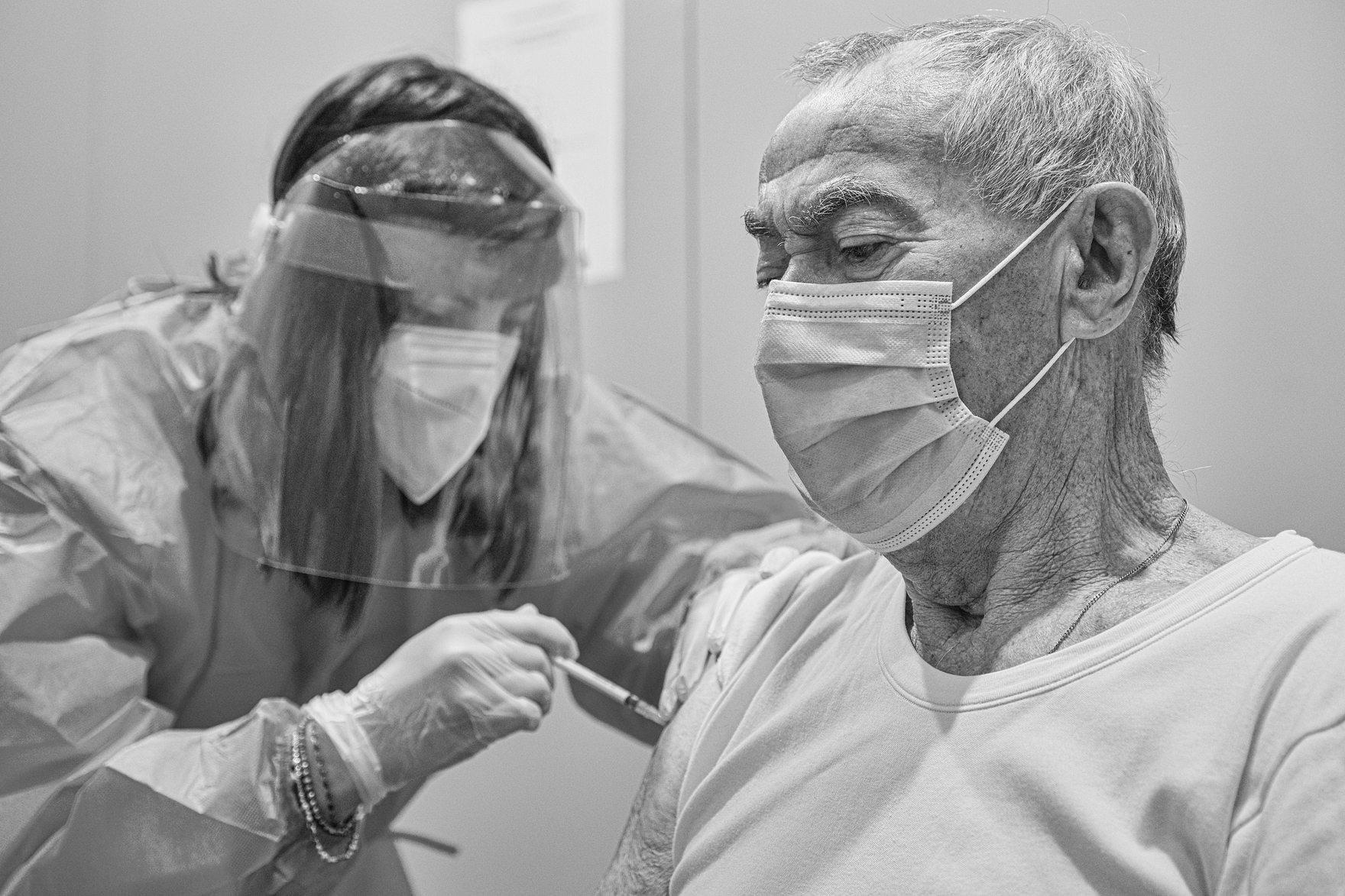
Consider the confusion of the vaccine rollout across Canada in 2021; we all had trouble booking vaccine appointments. Imagine how much more challenging it was for people who are either not tech-savvy or don’t have the wherewithal to possess or use smartphones, with sufficiently speedy internet connections. In particular, seniors, marginalized and rural populations were often left behind.
Data and digital technologies are powerful tools, but they have obvious limitations — including potential threats to privacy and data rights. A recent report by a Lancet and Financial Times commission flagged the need for a new “data solidarity” — in essence, a reframing of big data and its digital technologies as social goods, rather than as mere technical instruments. It’s a powerful idea.
We know that better data enables better research, which can contribute to healthier populations. But while data is indeed vital, we mustn’t forget that health care is ultimately about patients and their welfare. If we systematically aggregate data in a way that is calibrated to concretely improve patient health, that data will necessarily become better organized, more secure and more accessible to patients. Big data holds great promise in improving health outcomes but no amount of techno-enthusiasm can obscure the current lack of national or global standards around its collection, storage and use.
Looking beyond Canada, policy makers need to urgently consider how health care can be better planned, financed and administered to address global challenges. As the pandemic drags into its third year, we know that focusing on domestic concerns alone will never pull us out of it. In addition to a plentiful global supply of safe and effective COVID-19 vaccines, we must ensure that health systems around the world have access to timely data.
Good governance is essential for positive change. Data trusts — legal entities that steward individuals’ grouped data for designated purposes such as health research — are just one mechanism to extract benefits from personal data for the public good. We can broaden this. If international norms are created around the collection, storage and use of data, cooperation across countries can ensue, leading to ever-larger and diverse data sets accessible to medical researchers around the world. The potential social benefits are enormous.
Governments and health bodies can take the first, important steps forward by ensuring that their gathering of health data is always trained on better public health outcomes and better research. They need to do this in a manner that is patient-focused, inclusive and rigorous about protecting privacy. Where successes emerge, lessons learned should be scaled and shared across the country and around the world.
Comprehensive data reform will be neither easy nor inexpensive. But the cost of inaction is arguably much greater. In the absence of a truly patient-centred system, we risk leaving a large segment of society permanently on the periphery, looking in.
This article first appeared in the Toronto Star.